What is Revenue Cycle Management and Why Does it Matter?
Written by Erica Sobers
Revenue Cycle Management (RCM) is the process of utilizing medical billing software, that healthcare facilities use to track patient care episodes from registration and appointment scheduling to the final payment of a balance. (What is “Revenue Cycle Management“)
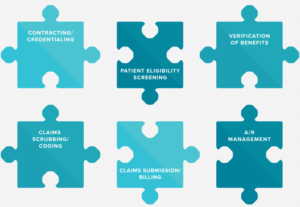
Financial management isn’t fun but it’s necessary for all healthcare organizations. Here at UPIC Health, we understand that cash flow is king. The “bottom line” is fundamental to every business. We are skilled and dedicated to eliminating as many barriers to care as possible for patients and providers alike. Most people only see one part of the process; patient scheduling, registration and payment collection. But that is just the beginning, as shown below, there are claims submissions, benefit verifications, and claims management. This helps to ease the process of maintaining financials and lets organizations focus on seeing patients.
Barriers to achieving an efficient RCM flow usually start at the front desk or when the appointment is made. Inaccuracies when collecting insurance information can cause huge issues including front desk staff thinking the patient does not have insurance, a lengthy verification process and patients being billed incorrectly and charged too much up front. Capturing patient data correctly is an essential component of the RCM process.
Having an efficient claims submission process can help detect costly errors in coding. Unidentified errors in the coding can result in patients being charged for services they did not receive or not being charged for services they did receive, leaving money on the table for the business.
Proper staff training, paying attention to detail and making sure no shortcuts are taken throughout the claims submissions process can all make a world of difference in the efficiency of the RCM process. At UPIC Health we are dedicated to making this process seamless for you.
Reach out for a free consultation today
Get StartedUPIC Hires Veteran Healthcare Operations Director
FOR IMMEDIATE RELEASE
Contact: Juli Briskman
Phone: 703 772-1148
Email: juli@UPICHealth.com
Twitter: @UPICHealth

Rick Sletten joins UPIC Health as Operations Director in Norfolk, Va.
NORFOLK, VA (Sept. 26, 2018) — UPIC Health, LLC recently hired Rick Sletten as Operations Director to lead the growing organization’s ongoing effort to improve and centralize healthcare delivery by aligning technology and resources to better serve UPIC clients and their patients.
“I chose to join UPIC because the organization’s pioneering strategy is the way forward in healthcare to maximize revenue and increase access,” Sletten said.
Sletten has more than 10 years of experience leading large health care operations most recently with Optum, a wellness company that serves more than 74 million customers as part of the UnitedHealth Group family of companies.
While at Optum, Sletten honed his revenue cycle management skills and created industry-leading processes governing front-end revenue operations including patient access and registration, charge entry & coding, service authorizations, time-of-service collections, scheduling. He is looking forward to advancing and modernizing these processes for UPIC clients.
“Rick’s experience has given him a national view into the intricacies of the revenue cycle process. He can identify the bottlenecks that hinder timely payments and remove them permanently,” said UPIC Health CEO, Mary Tucker. “We are thrilled to have Rick on board to shape the future of UPIC’s model for meaningful engagement in care. He will build on an already great foundation of service delivery as we continue to grow our services in the United States and globally.”
Sletten is a member of the American College of Healthcare Executives and the Healthcare Financial Management Association. He lives in Norfolk, Va. with his wife and toddler. To learn more about his experience in healthcare, visit his LinkedIn profile.
About UPIC
UPIC Health is a mid-size, privately-held company with operations in Chantilly and Norfolk, Va. A business process outsourcer, UPIC offers patient contact center, revenue cycle management, and telebehavioral health services to clients across the country, all practicing under the value-based reimbursement concept. UPIC is a 2018 Velocity Growth Award Winner and Growth Story of the Year. To learn more, visit our website at www.upichealth.com or email Chief Marketing Officer, Juli Briskman at juli@upichealth.com. Follow us @UPICHealth.
###
Reach out for a free consultation today
Get StartedUPIC Designated Top 10 Patient Engagement Solutions Provider
By Juli Briskman
Aug. 14, 2018
![]() UPIC Health is honored to be designated one of the Top 10 Patient Engagement Solution Providers for 2018. Each year Healthcare Tech Outlook publishes the Top 10 List based on reader feedback and editorial research of the industry.
UPIC Health is honored to be designated one of the Top 10 Patient Engagement Solution Providers for 2018. Each year Healthcare Tech Outlook publishes the Top 10 List based on reader feedback and editorial research of the industry.
“We are so pleased that an organization based on empathy is being recognized for outstanding service,” said UPIC CEO, Mary Tucker. “Empathy, Engagement, and Efficiency are what we believe in and we combine the three of them to ensure patients get the best possible care.”
This year has brought several accolades to UPIC, which has grown six-fold mainly through referrals since launching four years ago. UPIC received the 2018 Velocity Growth Award from CEO Report Baltimore and CEO Washington, D.C. Earlier this year, Tucker was featured on What’s Working Washington and was named to the SheSource database by the Women’s Media Center as an expert in Healthcare.
“This is no time to rest on our laurels,” Tucker says. “We are expanding into mental health counseling with our video social work application and continue to grow our outsourcing business in contact centers and revenue cycle management. 2019 is poised to be our best year yet.”
UPIC Health is a mid-size, women-owned and operated, private organization with operations in Chantilly and Norfolk, Va. A business process outsourcer, UPIC offers patient contact center, revenue cycle management, and telebehavioral health services to clients across the country, all practicing under the value-based reimbursement concept. UPIC is a 2018 Velocity Growth Award Winner and Growth Story of the Year recipient. To learn more, visit our website or email Chief Marketing Officer, Juli Briskman at juli@upichealth.com. Follow us @UPICHealth.